Parasites In Humans
Find The Nastiest Parasites In Humans
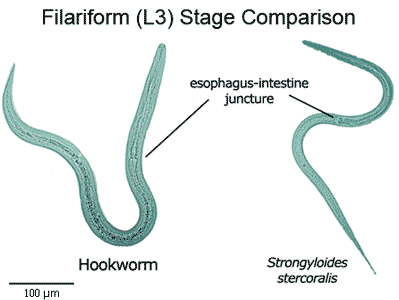
HookwormsHookworms are bloodsucking roundworms living in the small intestine. Some common names for hookworm infections are: ancylostomiasis, necatoriasis, Egyptian chlorosis, tunnel disease, miners' anemia and brickmaker's anemia. Hookworms are the second most common human worms (the most common is Ascaris lumbricoides). There are thousands of hookworm species but only two of them target humans. Necator americanus (necatoriasis) and Ancylostoma duodenale (ancylostomiasis) infect over one billion people around the globe mostly in tropical and subtropical climates. Necatoriasis predominates in the Americas (North, Central and South America) and Australia, whereas ancylostomiasis occurs in the Middle East, southern Europe and North Africa. Necator americanus is gray-pink in colour. Male is 5–9 mm and female 10 mm long and about 0.5 mm thick. Usually they live a few years but can live up to 15 years. Females produce up to 10 000 eggs per day. Necator americanus is very similar to Ancylostoma duodenale. Ancylostoma duodenale males are 5–10 mm and females 10 mm or more in length and 0.5 mm thick. They live only about six months. Females produce up to 30 000 eggs per day. The hookworm larvae that start the infection are less than a millimeter long. These third stage, L3, larvae called filariform live on warm moist soil that has been contaminated with infected human feces. Upon touch, a tiny filariform larva attaches to the skin and penetrates it. It burrows through tissue until it reaches a blood vessel or lymphatic duct. It travels in the bloodstream to the small pulmonary capillaries. It breaks into the lung alveoli and is taken towards the bronchus and trachea by the movement of microvilli. It is coughed up to the throat and swallowed through the esophagus to the stomach. After passing the stomach it hooks into the intestinal mucosa in the small intestine and starts sucking blood. The arrival to the small intestine takes about a week. Then within a few weeks it develops into an adult and is ready to mate. The produced eggs exit the body in the feces. Rhabditiform (first stage, L1) larvae hatch in the feces or in warm, moist, sandy soil within two days. They feed on organic matter and grow rapidly. They molt twice within 10 days to become filariform (third stage, L3) larvae that are infective. Filariform larvae can survive up to four weeks in the right conditions (warmth, moisture, shade). Although most hookworm larvae travel straight to the small intestine, sometimes larval Ancylostoma duodenale migrate to muscle tissue and become dormant. These sleeping larvae make up a reserve that can cause infection years after treatment. According to some reports filariform larvae of Ancylostoma duodenale can cause infection, if ingested. So in theory it is possible to get infected by accidentally swallowing contaminated dirt. Necatoriasis on the other hand always requires migration through the lungs.
Infected humans are more often adult men who work barefoot on fields. Hookworm infection is the most problematic for women and children. Women lose blood with menstrual flow once a month. They also need extra nutrients for babies. In some developing countries 30 % of pregnant women are infected with hookworms. Their newborn babies might have low birth weights or even die. When a woman gives birth, she excretes certain hormones into the bloodstream. The sleeping larvae (only Ancylostoma duodenale) in the muscles wake up and find their way into the mammary glands. When the mother breastfeeds her baby, the child gets infected, too. Hookworms can cause some of the following symptoms:
Diagnosis of an intestinal hookworm infection is done by identifying hookworm eggs from a stool sample under a microscope. Another stool sample after treatment is often required to make sure all hookworms are dead. The infection is usually treated for 1–3 days with medication prescribed by your health care provider. Some good drugs against hookworms are benzimidazoles such as albendazole and mebendazole. The drugs are effective and appear to have only few side effects. Iron supplements may also be prescribed to cure anemia. Despite of all efforts, the infection might still continue due to awakened dormant larvae or new infections. Hookworm infection is rarely lethal. In fact, hookworms have been used to cure autoimmune diseases. In helminthic therapy hookworms are voluntarily swallowed. The parasitic infection prevents the overly active immune system from destroying tissue focusing only on the foreign organisms. Human feces should not be used as fertilizer in agriculture. Do not walk barefoot or touch soil in areas where hookworms are common. Also if you have cats or dogs, treat them with anti worm pills regularly. Cutaneous larva migransAnimal hookworms Ancylostoma braziliense and Ancylostoma caninum normally parasitize only dogs and cats. In humans they cause a skin condition called cutaneous larva migrans, creeping eruption or ground itch. In the canine (or feline) intestine a female hookworm releases eggs into the stool. The feces land on soil, and rhabditiform larvae hatch and evolve into filariform. The filariform larvae burrow into human skin and start migrating in the epidermis. They cannot usually breach the subcutaneous layer and live only up to a few months. They can migrate several centimeters per day causing itchy red lesions and vesicles on the skin.
Cutaneous larva migrans is usually diagnosed from the signs and symptoms without laboratory tests. There are no serologic tests for animal hookworm infections for humans. Cutaneous larva migrans is a self-limiting infection and does not always require treatment. Severe cutaneous larva migrans infections can be treated with albendazole and surgical removal. Sometimes larval Ancylostoma caninum is able to penetrate the lower skin layer and migrate to the small intestine, causing eosinophilic enteritis. It is possible that it can also migrate to the eye and cause diffuse unilateral subacute neuroretinitis (DUSN). At the early stage of DUSN it might cause vitritis, visual loss, mild papilledema, and consecutive crops of multiple, evanescent, deep, gray-white, retinal lesions. After several months there might be widespread, diffuse and focal depigmentation of the pigment epithelium, retinal arterial narrowing, severe visual loss, optic atrophy, and electroretinographic changes.
Rhabditiform larva of a human hookworm is about 0.3 mm long.
Filariform larva of a human hookworm is about 0.6 mm long.
Also check out the videos. Hookworm QuizTo reveal the answer you need to click the correct option. How long do hookworms live?+ A) A few days
+ B) A few months
+ C) A few years
|
Parasites In Humans Pictures And Videos Contact Info Privacy Policy Sitemap
© 2010–2015 parasitesinhumans.org






 Does cutaneous larva migrans always need to be
treated?
Does cutaneous larva migrans always need to be
treated?